RURAL CANADA: ACCESS TO HEALTH CARE
If there is two-tiered medicine in Canada, its not rich and poor, its urban versus rural.(1) This is how Health Canadas Special Advisor on Rural Health described the increasingly dire circumstances facing rural Canadians with respect to access to health care. It has been shown that the health status of rural residents is lower than that of their urban counterparts. At the same time, rural Canadians are limited to a smaller range of health care providers; rural hospital closures and centralization of health services have had a severe impact on rural residents.
This paper presents the issues and challenges of providing health care in rural Canada and examines the role, both existing and potential, of the federal government in this area.(2) It begins by presenting the demographic and economic characteristics of rural Canada and looking at the health status and needs of rural Canadians. It then examines the issues of access to care and the supply of human resources in health care in rural areas. Finally, possible strategies and solutions to the problems of access to health care in rural Canada are discussed. The paper concludes with an appendix outlining some of the approaches to rural health taken by the United States, Australia and the United Kingdom, and possible lessons for Canada.
RURAL CANADA: FACTS AND FIGURES
Canadas rural population appears to be in decline,(3) dropping from just over 8.6 million people in 1991 to some 6.1 million in 2001. In contrast, as of 2001, 79.7% of Canadas total population lived in urban centres up from 68.4% in 1991.
There are significant variations in urban/rural distribution among the provinces and territories (see Figure 1 and Table 1). For instance, in British Columbia and Ontario, only 15.3% of the population lived in rural areas in 2001, while in the Atlantic provinces, rural residents made up between 42% and 55% of the population. In Nunavut, 67.5% of the population lived in rural areas.
FIGURE 1
Distribution of Canadas Population by Urban and Rural, 2001
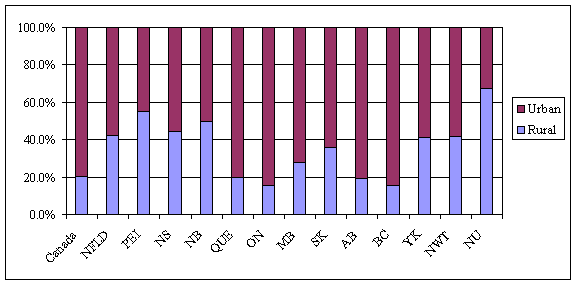
Source: Statistics Canada, 2001 Census, Population and Dwelling Counts, Urban and Rural.
TABLE 1
Canadas Rural Population, Distribution and Age
|
|
1991 |
2001 |
|||||
|
|
RURAL |
% |
MEDIAN(a) |
RURAL |
% |
MEDIAN(a) |
|
| Canada |
8,626,086 |
31.6 |
35.5 |
6,098,883 |
20.3 |
39.0 |
|
| Newfoundland and Labrador |
374,050 |
46.4 |
34.2 |
216,734 |
42.3 |
39.5 |
|
| Prince Edward Island |
85,624 |
66.0 |
34.5 |
74,619 |
55.2 |
37.9 |
|
| Nova Scotia |
509,520 |
56.6 |
36.9 |
400,998 |
44.2 |
40.5 |
|
| New Brunswick |
469,265 |
64.8 |
35.2 |
361,596 |
49.6 |
39.1 |
|
| Quebec |
2,040,936 |
22.4 |
36.3 |
1,420,330 |
19.6 |
40.1 |
|
| Ontario |
2,497,023 |
18.2 |
36.4 |
1,747,499 |
15.3 |
39.5 |
|
| Manitoba |
412,445 |
27.9 |
33.9 |
314,262 |
28.1 |
36.0 |
|
| Saskatchewan |
489,458 |
49.5 |
36.0 |
349,897 |
35.7 |
38.5 |
|
| Alberta |
715,605 |
20.2 |
33.0 |
569,647 |
19.1 |
35.3 |
|
| British Columbia |
874,909 |
19.6 |
36.3 |
597,885 |
15.3 |
40.2 |
|
| Yukon |
11,462 |
41.2 |
32.4 |
11,831 |
41.3 |
36.9 |
|
| Northwest Territories |
45,789 |
63.3 |
27.2 |
15,529 |
41.6 |
29.0 |
|
| Nunavut |
N/A |
N/A |
21.4 |
18,056 |
67.5 |
22.1 |
|
Source: Population: Statistics Canada, Census 1991, Urban Areas Population and Dwelling Counts, Cat. No. 93‑305, and 2001 Census, Population and Dwelling Counts, Urban and Rural; Age: Median Age, rural and small town areas, Canada, provinces and territories, 1996 and 2001 in 2001 Census Profile of the Canadian population by age and sex: Canada ages.
Notes: (a) The median age is the point
where exactly half of the population is older and half is younger.
(b) 1996 data.
Canadas population is aging rapidly. However, the population of most rural areas in Canada appears to be aging faster than that of urban centres. The median rural age increased by 3.5 years to 39 years between 1996 and 2001, while the median age in metropolitan areas increased by only 1.8 years to 37 over the same period.(4)
However, the ages of Canadas rural populations are not uniform throughout the country. The median ages in rural Nunavut and rural Northwest Territories were 22 and 29 years, respectively, for 2001. This is partly due to the Inuit population, which is young and growing rapidly because of higher birth rates. The rural populations of Nova Scotia and Newfoundland and Labrador experienced significant aging, relative to their metropolitan areas, between 1996 and 2001, with the migration of younger people to urban centres. These variations in population characteristics among the provinces must be taken into account in public policies aimed at rural health.
B. Economic Factors
In all provinces, incomes in rural regions are lower than in urban regions (see Table 2). However, this income gap has narrowed over the last two decades, decreasing by 16% between 1980 and 1995.(5) Nova Scotia and Manitoba had the largest urban-rural income disparities. As Table 2 also shows, the three provinces that had above-average urban incomes (British Columbia, Alberta and Ontario) also had above-average rural incomes.
TABLE 2
Per Capita Income and Unemployment Rates in Rural and Urban Areas
|
|
1995 Per Capita Income |
2000 Unemployment Rate(b) |
||
|
|
RURAL |
URBAN |
RURAL |
URBAN |
| Canada |
$16,120 |
$19,543 |
7.2% |
5.4% |
| NFLD |
12,736 |
15,456 |
22.0 |
8.8 |
| PEI |
15,316 |
N/A(a) |
16.7 |
7.8 |
| NS |
14,223 |
18,532 |
9.7 |
6.8 |
| NB |
14,887 |
16,838 |
12.0 |
6.4 |
| QUE |
14,792 |
17,696 |
8.9 |
7.0 |
| ONT |
17,585 |
20,696 |
4.3 |
4.7 |
| MAN |
14,638 |
18,164 |
3.9 |
4.1 |
| SASK |
14,916 |
17,985 |
4.2 |
4.3 |
| ALTA |
16,681 |
19,900 |
4.0 |
3.7 |
| BC |
17,957 |
20,832 |
7.4 |
6.0 |
Source: Per capita income: Vik Singh, Rural Income Disparities in Canada: A Comparison Across the Provinces, Rural and Small Town Canada Analysis Bulletin, Vol. 3, No. 7, Statistics Canada No. 21-006-XIE, 2002, Appendix Table 1.
Unemployment rate: Rural Neil Rothwell, Employment in Rural and Small Town Canada: An Update to 2000, Rural and Small Town Canada Analysis Bulletin, Vol. 3, No. 4, Statistics Canada No. 21-006-XIE, 2001, Appendix Table 1; Urban Statistics Canada, CANSIM II, Table 282-0066.
Notes: (a) According to the authors definitions, all of Prince
Edward Island is classified as rural.
(b) 2000 unemployment rate is for the 25 to 54 age
group.
Rural Canada has consistently had higher unemployment rates than the urban regions of the country(6) (see Table 2 for 2000 data). This is partly because seasonal work is more prevalent in rural areas than in urban ones. Month-to-month changes in employment and resources caused by seasonality make it difficult to sustain steady and long-term economic growth.(7) Rural unemployment rates also vary considerably among the provinces, ranging from 22% in Newfoundland in 2000 to 3.9% in Manitoba (again, this can be explained partly by the seasonality of dominant industries in rural regions the Atlantic provinces have an above‑average representation in fishing, which is the most seasonal of all industries).
Historically, rural Canada has been identified with primary sector employment. However, the rural industrial picture is changing quickly. Table 3 presents rural employment data by industry group for 1996 and for 2000, both as a percentage of total rural employment and in terms of its intensity relative to all of Canada.(8) It appears that traditional rural industries such as agriculture(9) and forestry, fishing, mining, oil and gas now account for a smaller share of total rural employment. Manufacturing, trade, health care and social assistance, educational services, accommodation and food services, transportation and warehousing, and the management of companies (not shown in Table 3) have increased in both importance and relative intensity in rural areas.
Overall, the rural workforce seems to be reducing its dependence on traditionally seasonal industries. However, the movement away from seasonal and primary sector employment and towards manufacturing, trade, transportation and social services could cause economic hardship for rural regions that have relied heavily on these former industries. Indeed, transitions to other industry groups may be extremely difficult for these regions.
TABLE 3
Rural Employment by Industry Group
|
|
1996 |
2000 |
||
|
|
As %
of |
Intensity |
As % of |
Intensity |
|
Manufacturing |
14.2 |
99.3 |
15.6 |
101.7 |
|
Trade |
14.1 |
90.4 |
14.3 |
92.3 |
|
Health Care and Social Assistance |
9.7 |
93.6 |
10.0 |
97.6 |
|
Agriculture |
12.1 |
381.4 |
9.2 |
369.3 |
|
Construction |
6.5 |
122.1 |
6.6 |
120 |
|
Educational Services |
6.0 |
89.2 |
6.1 |
92.9 |
|
Accommodation and Food Services |
5.8 |
90.8 |
6.1 |
95.2 |
|
Transportation and Warehousing |
5.0 |
99.5 |
5.6 |
107.4 |
|
Forestry, Fishing, Mining, Oil, Gas |
5.0 |
230.1 |
4.7 |
248.9 |
Source: Rothwell, (2001), Table 3.
Notes: (a) Employment level of industry within rural area as a percentage of total employment in rural area.
(b) Using location quotients, this measures the intensity of employment in a specific industry within rural areas, relative to employment in that industry in Canada as a whole. A value of 100 indicates an equal degree of intensity between rural areas and Canada as a whole.
C. Health Status and Health Care Needs
The objective of Canadas health care policy, as enunciated under the Canada Health Act, is to protect the physical well-being of all Canadians and to provide all residents with reasonable access to health services without barriers.(10) Health status, however, is not evenly distributed across Canadas communities.(11) Life expectancies for rural regions are shorter than the Canadian average, and life expectancies among the remote northern communities are the lowest in the country.(12) In addition, residents of rural regions report having only fair and poor health more often than the Canadian average. In terms of lifestyles, the rates of smoking, heavy drinking and obesity are all higher in rural areas than elsewhere in the country.(13)
A number of studies have documented urban-rural differences in the areas of health status, lifestyles and patterns of health care use. These studies indicate that there is:(14)
-
A much higher prevalence of heart disease in northeastern Ontario;
-
Higher prevalence of certain types of cancer among farmers and miners;
-
Higher rates of long-term disability and chronic illness among rural residents;
-
Substantially higher rates of diabetes, respiratory and infectious diseases in Aboriginal communities;
-
Suicide rates among Inuit youth that are the highest in Canada;
-
More accident- and violence-related deaths and injuries in rural communities; and
-
Higher infant mortality in rural and small communities.
Indeed, the Office of Rural Health at Health Canada explains:
Rural realities and health needs differ from those of urban areas. These needs may be particular to the environment (e.g., the need for education on tractor roll-over prevention), changing demographics (e.g., an increase in the seniors population in some rural areas), a common health need present in a rural environment (e.g., the health status of First Nations communities), or the need for health concerns to be expressed in a rurally sensitive way (e.g., obstetrical services that do not generate an excessive travel burden on rural women).(15)
Information suggests that the health care needs of certain groups are often not met, nor are they always understood, in rural environments. The diversity of populations in rural and remote areas poses significant challenges to the health care systems in these regions. Increasingly, rural health experts insist that health care must acknowledge factors such as gender, age, occupation, environment, and cultural background as determinants of health; in turn, these factors should help to determine the range of services that should be provided in these communities.(16)
Generally, reports on rural health issues tend not to analyze health status by gender. Yet, women have more frequent and intimate contact with the health care system than do men. Contact with the system for women is often related to reproductive health and maternity care. They may require special health services to deal with problems relating to menstruation, birth control, unintended pregnancies, sexually transmitted diseases, infertility, childbirth, and menopause. However, access to gynaecological, obstetrical, and maternity services is decreasing outside of urban centres, and these services are often not readily available to women in rural regions. With respect to childbirth, it is becoming more and more difficult for rural women to deliver in their community, even if it has a hospital. In northern Ontario, the reported number of community hospitals that have closed their maternity ward has increased five-fold since 1981.(17)
Female cancers, particularly breast, ovarian and cervical cancer, raise the issue of the availability of cancer treatment facilities in rural regions. Low participation by women in screening programs is also a concern. Recent information shows that screening rates are markedly lower among rural women and women in poor socio-economic circumstances.(18)
Furthermore, women are disproportionately affected by social factors such as poverty and violence. Researchers from the Prairie Womens Health Centre of Excellence noted that:
the urban bias of specialized services for family violence, combined with the centralization of more generalized services such as Social Services, Legal Aid, and some aspects of the police service creates a serious issue of accessibility for rural women and their families. As a result women in rural areas must either find the resources to travel for these services or forego [sic] them. Women who leave abusive situations are often impoverished and may not be able to afford the time or the money to travel to the larger urban centre. Women in rural areas are also disadvantaged by the lack of subsidized daycare, inadequate employment opportunities, and lack of access to affordable housing.(19)
Young children, adolescents and seniors are often over-represented in rural regions. These age groups present unique challenges to the health care systems of rural areas. Health promotion and education for children and adolescents tend to be underdeveloped in many rural communities. Rural youth would benefit from early exposure to information on matters such as healthy diets and fitness, healthy sexuality, and the dangers of smoking, alcohol and drug abuse. Furthermore, abused children and adolescents in rural areas face geographical isolation, lack of information, lack of mobility, and possibly inadequate support services.
Seniors are the largest consumers of health care, primarily because they are more prone to disability and disease. In terms of mental health, depression is a prevalent concern among older adults. Isolated and rural seniors, in particular, often face barriers that impede their ability to maintain good mental health. With respect to physical health, elderly Canadians are more susceptible to malnutrition, osteoporosis, reduced sight and hearing, and other physical impairments, which can severely reduce their mobility. According to Statistics Canada, on average, residents of rural regions have the lowest disability-free life expectancy in Canada.(20) In regions such as the Atlantic provinces, where there is considerable rural emigration by younger individuals, more and more rural seniors may be left alone to cope with health problems.
Rural regions must often struggle for economic survival. Geographic isolation, a reliance on natural resources, chronic high unemployment, and the vulnerability of single-industry towns can pose significant economic challenges to many communities. Furthermore, the economic activities on which these rural communities depend can have negative impacts on health. A number of occupations with a high concentration in rural areas, such as forestry, fishing, mining, farming, and the meatpacking industry, face important health concerns.
Forestry and fishing, for example, continue to be among the most hazardous industrial sectors. High accident rates, high incidence of occupational diseases and early retirement among workers are common in both industries. While mining has become increasingly safe since the 1960s, constant exposure to silica and radiation has resulted in silicosis and lung cancer among many miners.(21) Mine conditions may also be responsible for a much wider variety of obstructive pulmonary diseases and cancers of the bowel, stomach, bone, bladder and pancreas.
It has been reported that the occupation of farming represents more risks to health than any other industry in Canada.(22) In 2000, approximately 9.2% of the rural workforce was employed in agriculture (see Table 3, above). For the most part, farmers work in isolation on large plots of land, which means that few neighbours and few services are readily available. Farmers are exposed to heavy and hazardous equipment and to a wide variety of noxious substances such as pesticides. Furthermore, the farm is both a workplace and a home, meaning that children and seniors may also be exposed to the same health and safety risks. While other hazardous occupations are usually regulated and their workers protected against dangerous working conditions through legislation, in farming, due to the prevalence of independent owner/operators, health and safety regulations may not be given sufficient consideration.
Recently, the number of self-employed farmers with no employees has dropped significantly, and there has been a move toward larger farms.(23) Rapid expansion of intensive cattle and hog feeding operations has been encouraged, especially in Alberta, by government incentives and a favourable labour climate (there is a relatively low level of unionization in the meatpacking industry). The meatpacking industry is characterized by hazardous work environments, low pay and a high employee injury rate (in Alberta, the rate of injury claims was double the provinces average for manufacturing in 1996).(24) A high rate of injuries places an immediate demand on a regions health care system. Moreover, according to a recent study, meatpacking towns can be plagued by other, less visible, health issues. Due to the nature of the work, companies tend to recruit young adult single males, many of whom arrive from out of province. In addition to having to deal with a new community and stressful working conditions, this demographic group is highly susceptible to alcohol abuse and related problems. It has been shown that the rapid expansion of meatpacking operations into rural communities seems to exacerbate the occurrence of alcohol abuse and domestic violence.(25) It is difficult for small rural towns to meet these demands, due to shortages of qualified health care personnel.
There is quite often a conflict between regional economic growth and regional health in rural areas. For example, intensive livestock operations (feedlots or factory farms) play vital roles in the economies of certain provinces (most notably Alberta, where 60% of Canadas feed-cattle production takes place) and in the lives of many rural residents. While these operations hold great importance for the economies of small and rural towns, they can pose a threat to a regions water supply, air and soil quality, and overall health of residents. Feedlot Alley, a 500-square-kilometre area near Lethbridge, Alberta, has the densest concentration of livestock anywhere in Canada. This region has experienced remarkable economic expansion: in the past 20 years, livestock operations have grown three times in size. However, the Chinook Regional Health Authority, which services Feedlot Alley, reported one of the highest rates of gastro-intestinal illnesses in Alberta in 1998, with rates one and a half times the provincial average.(26) When compact areas are crowded with hundreds of thousands of livestock (it is estimated that Feedlot Alley is home to 520,000 cattle and 180,000 hogs), the danger of manure and the bacteria, parasites and phosphorus it contains getting into local lakes, rivers and underground aquifers becomes a serious health concern. Recent water-contamination tragedies in North Battleford, Saskatchewan, and in Walkerton, Ontario, demonstrate that these threats are very real.
Over 50% of Aboriginal Canadians live in rural communities. Their health, in comparison to that of the population as a whole, is relatively poor. Health indicators include higher prevalence of many chronic diseases, suicide, alcohol and substance abuse, family violence, and communicable diseases, to name but a few.
HEALTH CARE PROVIDERS AND ACCESS TO CARE IN RURAL CANADA
A. Physician Distribution
Physicians are not evenly distributed throughout Canada. This unevenness is particularly serious in rural and remote areas. The problem also appears to be worsening: in 1991, 14.9% of Canadas physicians practised in rural areas; by 1996, this number had dropped to 9.8% (see Table 4). Perhaps more important, this decline in rural physicians has occurred at a greater rate than the decline in Canadas rural population.(27) Furthermore, according to projections, the ratio of physicians per 1,000 population in rural areas is expected to decrease from 0.79 in 1999 to 0.53 by 2021.(28)
TABLE 4
Physicians and Population in Rural Areas
|
|
% of Population Living |
% of Physicians Practising |
| 1991 |
29.2% |
14.9% |
| 1996 |
22.2% |
9.8% |
Source: Pitblado and Pong (1999), p. 3.34.
A number of experts stress that, while these data are distressing, physician/population ratios have major limitations: these ratios fail to take into consideration differences in physician productivity, mobility of both physicians and patients, substitution by other health care providers, and the medical needs of the population.(29) These experts suggest that another method of analyzing the distribution problem (called the Gini index) might be used to determine how equitably physicians are distributed spatially.
The Gini index compares the proportion of physicians to the proportion of the population in the same geographical area. Gini values range from 0 to 100, with 0 representing perfectly equitable distribution and 100, total inequality (all the countrys physicians being located in one neighbourhood). Therefore, smaller values of the Gini coefficient indicate a more equal geographical distribution of physicians and population. Table 5 compares the distribution of numbers of physicians and the numbers of people among census divisions in Canada by reporting Gini indices, ranked by physician specialty.
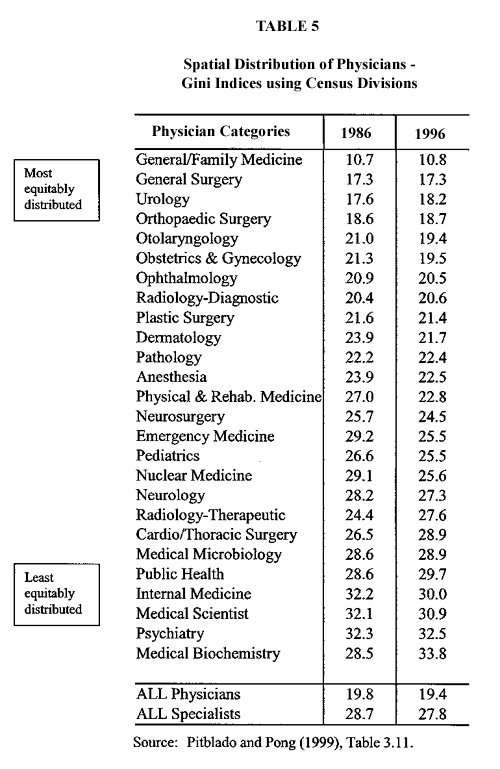
General/family physicians were the most equitably distributed category of physicians among census divisions. As for medical specialties, general surgery was the most equitably distributed in 1996, while medical biochemistry was the least.
Most rural health researchers agree that the distance to health care providers and facilities is increasing for rural residents as physicians and hospitals become more concentrated in urban and urban fringe areas.(30) According to a recent study, more than two-thirds of residents of remote northern communities live more than 100 kilometres from the nearest physician.(31)
Most medical specialties are inequitably distributed throughout the country. Dr. Stuart Iglesias, a physician from rural Alberta, has observed that graduates of specialties such as surgery and obstetrics are not interested in working in rural community hospitals the volume and complexity of cases is low and the proportion of night and weekend calls is excessive. As a result, family physicians and general practitioners are required to perform a wide range of procedures; for example, family physicians rather than obstetricians attend most rural deliveries.(32) There is concern that if rural regions continue to lose specialists, the hospitals that serve these residents will no longer be able to offer comprehensive care and will face the prospect of providing little more than ambulatory care and transportation services to urban health care facilities.(33) Although this situation will be mitigated as improvements in the application of telehealth technology reduce the need to travel, the loss of self-sufficiency and local capacity in rural areas remains problematic. The Secretary General and C.E.O. of the Canadian Medical Association explained that we understand that, in certain cases, you cannot make a business case for providing reasonable access to people living in rural and remote areas. However, you may actually have to say that while it may not be cost effective, it is the right thing to do.(34)
In the summer of 2001, an editorial letter appeared in The Globe and Mail entitled Why I will refuse to be a rural doctor.(35) The author, a young medical school graduate, explained that, despite having grown up in a small town, he is now city folk, his habits are city habits, [his] life is a city life. He went on to say:
The men and women in my medical class are much like me. Many are interested in rural medicine, but in the end few will work in towns of fewer than 50,000 people. They have or want partners with careers of their own. They want time away from work. They have spent 10 years or more at an urban university and are accustomed to the conveniences of urban life. That is why the physician shortage in rural Canada will not be fixed any time soon. Young doctors and their partners are not willing to make the sacrifices to go to a rural community.
This letter illustrates the significant barriers faced by rural areas in recruiting and retaining physicians barriers that consist primarily of differences in lifestyle and that remain resistant to government policy intervention. Physicians, facing decisions about where to practise, consistently rank personal factors as the most important considerations. A recent survey of the reasons why some physicians left rural regions in Ontario concluded that spousal contentedness, child-related issues and social isolation were areas that should be explored in attempting to retain physicians on a long-term basis in rural locations.(36)
Rural areas difficulty in attracting physicians also has to do with professional considerations. Rural practice is different from urban practice. With fewer physicians, rural family doctors typically work longer hours than their urban counterparts; with fewer specialists, rural doctors are also obliged to provide a much more comprehensive range of services: on-call, emergency care, hospital in-patient care, and childbirth care, for instance. Other professional considerations include relatively less accessible professional support (colleagues and specialists), fewer facilities, equipment, and supplies, and difficulty in pursuing continuing training and educational opportunities.
It has been argued that a third set of reasons relates to recent licensing and training policies of provincial/territorial authorities.(37) Because of the smaller population of rural communities, the majority of physicians are general and family practitioners; often smaller communities just do not have sufficient population to justify medical specialists. Due to the wide range of their knowledge and skills, general/family practitioners are often considered to be the best suited for the overall health care needs of residents. Hence, an increase in the number of medical graduates choosing medical specialties at the expense of general/family practice will most likely have a significant negative impact on rural areas. In the early 1990s, provincial/territorial licensing authorities, based on advice from the Federation of Medical Licensing Authorities and the College of Family Physicians of Canada (CFPC), decided to replace the rotating internship with a two-stream choice: either a specialty residency leading to Royal College certification, or a two-year family practice residency leading to CFPC certification. The effect of this policy decision seems to have been that fewer residents overall are channelled into the family practice stream. First, under the two-stream model, an additional year of training is now required for those who choose family practice. Second, the elimination of the rotating internship seems to be forcing young physicians to decide on a career specialty earlier than previously. Finally, some maintain that the physicians who were produced through the rotating internships received a wider range of exposures and experiences and were better equipped to handle the breadth of situations faced by rural practitioners.
According to two health policy researchers, the effect of these policy-based changes on the recruitment of rural physicians may be relatively small; nevertheless, it is significant:
Prior to the elimination of the rotating internship, about 900 new Canadian-trained physicians were entering general practice. With the advent of the family practice two-year residency requirement, it appears that about 700 new Canadian-trained physicians now enter general practice annually. On average, about 15-20% of new family practitioners establish practices in rural or remote areas each year. Thus, although the graduating complement has fallen by about 200, one would expect the reduction in those likely to take up rural or remote practice opportunities to have declined by about 30-40 per year, for the country as a whole.(38)
In an attempt to maintain adequate access to health care for residents of rural regions, the provinces and territories have generated an array of strategies and incentive programs to entice physicians to rural and remote areas and to encourage them to stay there. According to Barer and Wood, provincial policies may be grouped into four main categories: regulatory/administrative, educational, financial, and laissez-faire or market solutions.(39)
-
Regulatory/administrative approaches include policies used to influence the location decisions of physicians through laws and regulations. Restricting the issuance of billing numbers in urban areas, so that physicians cannot be reimbursed by the provincial health care insurance plan, and implementing controls on the licensing of foreign medical graduates, are both examples of regulatory/administrative approaches. These types of approaches, however, were found to be in contravention of the Charter of Rights and Freedoms; it has been difficult, therefore, to assess their impact on the problem of physician distribution.(40)
-
Educational initiatives include a wide range of policies, from enriching high school science classes in rural areas to increased emphasis on rural medicine in Canadian medical schools. This area is only beginning to be explored in any depth by provincial/territorial governments, and might have considerable potential. Since it has been established that medical graduates who have grown up in rural areas are more likely to come back to practise in these areas, exposing rural high school students to the health care profession or admitting more medical students from rural areas could have positive effects on these regions. This initiative is discussed further in the section of this paper that reviews possible strategies and solutions.
-
Financial approaches, which consist of different methods of payment and incentives to health care providers, are the most commonly used policy strategies. These include guaranteed minimum income contracts, northern/isolation allowances, loan forgiveness, assistance with practice expenses, and differential fees (for instance, discounted fees for practitioners locating in oversupplied areas also known as urban disincentives). Some examples of recruitment programs include British Columbias $10,000 signing bonus to new rural doctors(41) and Ontarios Free Tuition Program, which provides up to $40,000 to final-year medical students, residents and newly graduated physicians in exchange for a full-time return-of-service commitment in an underserviced area in the province.(42) Because personal factors are known to have the greatest influence on location decisions, however, it has been argued by health policy experts that financial incentives have had little effect in correcting the shortage of physicians in rural areas.(43)
-
Finally, the laissez-faire approach involves relying on market forces: as urban centres become oversupplied with physicians, new physicians will slowly begin to set up in rural areas. Recruitment fairs aimed at attracting physicians for rural practice also fall into this category.
In their 1999 survey of provincial policy initiatives designed to improve access to necessary health services in rural regions, health researchers Barer, Wood and Schneider made the following observations:
While all regions of the country have some policies in place intended to improve access to medical services in rural and remote areas, there appears to be virtually nothing of a pan-Canadian nature in place. This is undoubtedly in large measure due to the fact that health is, constitutionally, a provincial/territorial matter. As a result, there are relatively few policy levers held at the federal level (immigration policy being the one significant exception). Less immediately explicable is the vacuum in national (as distinguished from federal) policy. All provinces and territories face the same issues, and find themselves, instead, trying many of the same general policy approaches, with local colour added. This can become circular, and insular. The failure to develop any pan-Canadian initiatives has meant a history of destructive competition rather than co-operation. The solutions to issues of access in rural and remote areas would seem largely beyond the reach of any single jurisdiction.(44)
C. The Role of Foreign Medical Graduates
Rural Canada has relied heavily on the graduates of foreign medical schools to provide primary and advanced procedural care to its citizens. Every year, roughly 400 foreign‑trained physicians come to Canada. Partly because of conditional licences or other restrictions, many of them end up practising in rural and remote communities.(45) In fact, over half of the rural doctors in Saskatchewan are foreign-trained.(46) With respect to advanced surgical skills (specialists), approximately one-half of Canadas rural general-practitioner surgeons and one-third of general-practitioner anesthetists have been trained elsewhere. Of these foreign graduates, the largest group were trained in South Africa.(47)
While foreign medical graduates fill an important skills gap in rural Canada, some have argued that this cannot be a long-term solution; eventually, Canada must develop a self‑sustaining physician national plan for rural Canada.(48) Others call instead for not only a continuing reliance on foreign medical schools but also increased acceptance of international medical graduates, simply because policy options intended to achieve self-sufficiency will take too long.
D. Other Health Care Providers
While the distribution of physicians receives the greatest attention in the literature on rural health, it is widely accepted that other health care providers are also in high demand. Nurses and nurse practitioners, occupational therapists, physiotherapists, speech language pathologists, audiologists, and chiropodists are consistently sought after at rural recruitment fairs and tours. In fact, increased use of non-physician personnel could help significantly to alleviate the desperate physician shortages in many regions and improve access to primary health care for these residents.
The expanded deployment of such personnel could also provide a source of relief and on-call coverage for over-stretched rural physicians. However, much as with physicians, recruiting and retaining other health care providers is challenging.
POSSIBLE STRATEGIES AND SOLUTIONS
Telehealth refers to the use of information and communications technologies (ICTs) in the field of health care. The purpose of telehealth is twofold: to share health-related information among various health care providers and health care settings; and to deliver health services over large and small distances.(49) Many experts agree that telehealth, by supplementing the skills and knowledge of existing rural health care providers, is a very important part of delivering improved health care to rural residents.
Provincial and territorial governments have also been enthusiastic about telehealth projects and, with the assistance of the federal government (mainly through the Canada Health Infostructure Partnerships Program), are in the process of developing and expanding telehealth sites across the country.
Telehealth has important benefits for both patients and health care providers in rural areas. For the patient, telehealth provides for greater access to medical specialists, allows for quicker and more accurate diagnosis and treatment, and reduces travel time and costs. For the rural health care provider, telehealth decreases professional isolation and increases opportunities for continuing education. The Society of Rural Physicians of Canada warns, however, that telehealth must not be a substitute for local expertise: the enthusiasm for improved telecommunications and information technology must not divert resources so that rural communities are solely dependent on health care skills outside the region.(50) Furthermore, the technology must be of use to the community. For example, even with the equipment available, if the health care providers of a rural community are unfamiliar with digitizing X-rays and sending them electronically over a network, telehealth is of little help and the money is wasted.
According to the 2000 Rural and Remote Health Conference held at the University of Northern British Columbia, current public policy has not always been able to recognize the unique challenges of providing health services to rural and remote communities, due to insufficient research. First, there is a lack of basic data and information about rural health; most of the current health research is done in urban settings and is often inapplicable to rural communities. Second, any research that has been done has not been linked to public policy.(51)
Most rural health experts agree that rural health research can make significant contributions by: 1) helping communities and residents clarify health issues and take action on them; and 2) assisting at all levels in the development of rural friendly health policies. It has been argued that efforts at research have been fragmented, uncoordinated and have had little impact on policy.(52) Recently, a number of initiatives have attempted to provide an integrated approach. In 2001, it was announced that the Canadian Institutes of Health Research (CIHR), Canadas federal agency for health research, would provide $1 million to fund a number of studies that will provide diagnostic information about the state of rural health in Canada.(53) CIHR has stated that it considers rural health as a priority area for investment and that the agency would soon be developing a long-term rural health agenda. In addition, since 1999, CIHR has provided funding for the Canadian Rural Health Research Society (formerly the Rural Health Research Consortium), which was established as a twelve‑university initiative with the objective of strengthening Canadas capacity for research on health issues in rural areas.(54)
C. Rural Health Training and Education
It has been said that the current educational system produces rural doctors by accident and not by design.(55) Medical schools select people primarily from urban neighbourhoods and train them in an urban environment that promotes and emphasizes sub-specializations, research and academia. Graduates, consequently, have greater interest in sub-specialization and urban practice. Increasingly, family medicine training positions go unfilled, and even those graduates do not possess the skills needed for rural practice. In the opinion of the President of the Society of Rural Physicians of Canada, Peter Hutten-Czapski, the current system of training physicians generally does not act on the fact that practical training in rural medicine is important and that applicants of rural origin are the most likely to practise in rural settings.(56)
Who, then, produces Canadas rural doctors? Data suggest that the school of graduation affects the probability of physicians moving to and staying in remote areas. Universities such as Memorial University in Newfoundland and Université Laval in Quebec consistently produce the highest proportion of rural doctors in the country, while the University of Toronto produces the lowest.(57) This is partly attributable to Memorials and Lavals rural focus throughout undergraduate and postgraduate training, and their drawing and active recruitment of undergraduates from rural areas. The University of Toronto only recently established an office for rural medical education (1999) and draws the vast majority of its students from urban backgrounds.
McMaster University and the University of Ottawa are also recognized for their rural‑oriented postgraduate family medicine programs. Since 1991, McMaster University has offered two years of family practice training at Family Medicine North, based in Thunder Bay, Ontario. The program, which is intended to train family physicians for rural practice with the goal of retaining these graduates in rural areas, combines academic sessions in Thunder Bay with clinical experience in rural communities throughout northwestern Ontario. In 2001, the Society of Rural Physicians of Canada awarded the program the Keith Trophy for high-quality rural training and retention of graduates in rural areas: half of Family Medicine North graduates (25 of 50) are practising in rural areas.(58) Northeastern Ontario Family Medicine Program in Sudbury, affiliated with the University of Ottawa, has similar aims. However, its rate of retention of graduates in rural areas is much weaker: in 1998, only 6 of the programs 50 graduates (12%) were practising in rural areas. Even the University of Ottawa, Northeastern Ontarios urban parent, produced a greater percentage of rural doctors (18%).(59)
D. Recent Recommendations by the Romanow Commission and the Standing Senate Committee
In the fall of 2002, two prominent studies on the future of the Canadian health care system were released: the final reports of the Standing Senate Committee on Social Affairs, Science and Technology (October 2002) and the Romanow Commission on the Future of Health Care in Canada (November 2002). The Standing Senate Committee also plans to hold specific hearings on the subject of rural health and to release a thematic report with detailed recommendations in 2003 or 2004.
Both the Senate and Romanow reports acknowledge that the important challenge of improving access to health care in rural Canada needs to be addressed. The reports focus on expanding the supply of health care providers in smaller communities, as well as expanding innovative approaches such as telehealth. Specifically, the Romanow Commission proposed that a Rural and Remote Access Fund be established, with initial funding of $1.5 billion over two years, to improve access to health care in rural communities. It would be used to attract and retain health care providers, to give physicians and other health care providers increased exposure to rural experiences as part of their education and training, and to support the expansion of telehealth approaches.
Although it is easy to summarize rural Canada as approximately one-fifth to one-quarter of the Canadian population spread over 95% of Canadas territory, there exists incredible diversity among rural regions, both demographically and economically. The populations of rural regions in Atlantic Canada are aging quite rapidly while rural regions in the north, partly due to high Inuit birth rates, are relatively young. In terms of economic activity, Atlantic Canadas rural regions face high unemployment rates compared to the rest of the country. By contrast, economic activity is relatively stronger in Ontario, Manitoba, Saskatchewan and Alberta.
It has been shown that inequalities do exist in the health status of Canadians and that, in general, the residents of rural Canada are in poorer health than the average Canadian. Recently, the federal government has shown a willingness to address this imbalance. The Office of Rural Health was established in 1998 to ensure that the needs of rural Canada are better reflected in national health policy. A number of other federal initiatives have focused on improving our knowledge and increasing the amount of research relating to the health status and health care needs of rural Canada an area that, according to rural health experts, requires attention.
Arguably the biggest challenge faced by rural Canada is the problem of access to health care providers. Increasing physician shortages in rural regions means that many residents must travel for care sometimes considerable distances. Medical specialists are also in great demand in rural areas, as they often determine the self-sufficiency of a community. Communities that lack specialists must rely on their general practitioners and other health care providers to perform a wider variety of tasks; they have a greater need for telehealth technology, and are often obliged to send their residents to urban areas for treatment and care.
Rural health experts have suggested that the federal government play a leadership role in the areas of research, technology, education and the coordination of provincial/territorial initiatives. While each provincial/territorial government has its own policies intended to improve access to health care in rural areas, many experts agree that a coordinated, national effort would be more effective at reducing the gap in health status and health care access that exists between urban and rural areas.
(1) Interview with Dr. John Wooton, New Office to Focus on Rural Health Issues, Farm Family Health, Vol. 7, No. 1, Spring 1999.
(2) For a discussion of recent federal action in the area of rural health, see Nancy Miller Chenier, The Federal Role in Rural Health, PRB 00-20E, Parliamentary Research Branch, Library of Parliament, Ottawa, 2000.
(3) This paper uses the Statistics Canada definition of rural: all areas outside of urban centres with a minimum population concentration of 10,000 persons and a population density of at least 400 persons per square kilometre. There is no universally accepted definition of rural; in fact, numerous definitions exist and are used by researchers. For an in-depth treatment of rural as a geographic unit, see J. R. Pitblado and R. W. Pong, Geographic Distribution of Physicians in Canada, Centre for Rural and Northern Health Research, Sudbury, 1999, p. 2.7; and Valerie du Plessis, Definitions of Rural, Agricultural and Rural Working Paper Series, No. 61, Statistics Canada, Ottawa, 2002.
(4) Statistics Canada, 2001 Census Profile of the Canadian population by age and sex: Canada ages, Sub-provincial.
(5) Vik Singh, Rural Income Disparities in Canada: A Comparison Across the Provinces, Rural and Small Town Canada Analysis Bulletin, Vol. 3, No. 7, Statistics Canada No. 21-006-XIE, 2002, p. 6.
(6) Singh (2002), p. 28.
(7) Katherine Marshall, Seasonality in Employment, Canadian Economic Observer, Vol. 12, May 1999, p. 3.1.
(8) Relative intensity refers to a given industrys concentration of employment in rural areas compared to that industrys employment concentration in all of Canada. Labour economists often use location quotients as a measure of relative intensity: a value of 100 indicates an equal degree of intensity between rural areas and all of Canada, whereas a value greater than 100 means that, relative to the entire country, there is a higher concentration of employment in a given industry in rural areas.
(9) The apparent loss of agricultural employment may be more a reflection of the method of statistical reporting. The Labour Force Survey categorizes workers by their main job. A sizeable share of individuals working in agriculture also have another job. An increase in individuals reporting their non-farm job as their main job will have a negative effect on agriculture employment figures.
(10) Canada Health Act, Chapter C-6, Section 3.
(11) See Margot Shields and Stéphane Tremblay, The Health of Canadas Communities, Supplement to Health Reports, Vol. 13, Statistics Canada, Catalogue 82-003, 2002.
(12) Statistics Canada, The health of Canadas communities, The Daily, 4 July 2002.
(13) Shields and Tremblay (2002), Table 2.
(14) Raymond W. Pong, Rural Health/Telehealth, The Health Transition Fund Synthesis Series, Health Canada, 2002, p. 2.
(15) See the "Frequently Asked Questions" on Health Canada's site.
(16) For a more detailed discussion of the under-servicing of special needs groups in rural areas, see Therese Jennissen, Health Issues in Rural Canada, BP-325E, Parliamentary Research Branch, Library of Parliament, Ottawa, 1992.
(17) Peter Hutten-Czapski, State of Rural Healthcare, Presentation to the Standing Senate Committee on Social Affairs, Science and Technology, 2001, p. 3.
(18) Jan Roberts and M. Falk, Women and Health: Experiences in a Rural Regional Health Authority, Prairie Womens Health Centre of Excellence, 2002, p. 16.
(19) D. J. F. Martz, and D. B. Saraurer, Domestic Violence and the Experiences of Rural Women in East Central Saskatchewan, Prairie Womens Health Centre of Excellence, 2000, p. ii.
(20) Shields and Tremblay (2002), Table 2. Disability-free life expectancy is defined as the number of years of life that a person can expect to live without activity limitation and outside of a health care institution.
(21) Elliott Leyton, Dying Hard: The Ravages of Industrial Carnage, Oxford University Press, Toronto, 1997, p. 11.
(22) Mary Smillie, Agriculture Health and Safety: Prevention and Promotion, Health Transition Fund (Health Canada) Project SK325, 2001, p. 2.
(23) Statistics Canada, Farmers leaving the field, The Daily, 22 February 2002.
(24) Michael J. Broadway, Message in a Bottle: Community Health Issues for Meatpacking Towns, Health in Rural Settings: Contexts for Action, University of Lethbridge, 1999, p. 69.
(25) Broadway (1999), p. 80.
(26) Mary Nemeth, Raising a Big Stink, Macleans, Vol. 111, No. 32, 10 August 1998, p. 16.
(27) Pitblado and Pong (1999), p. 3.34.
(28) Hutten-Czapski (2001), State of Rural Healthcare, p. 1.
(29) Pitblado and Pong (1999), p. 2.6.
(30) Pitblado and Pong (1999), p. 4.3.
(31) Judith Kulig, Consortium for Rural Health Research, Evidence before the Standing Senate Committee on Social Affairs, Science and Technology, 31 May 2001, Issue 17.
(32) Neal Stretch and C. Knight, Community obstetrics: a new look at group obstetrical care in rural communities, Canadian Journal of Rural Medicine, Vol. 7, No. 3, Summer 2002, p. 183.
(33) Stuart Iglesias, The future of rural health: Comprehensive care or triage? Canadian Journal of Rural Medicine, Vol. 4, No. 1, Winter 1999, p. 33.
(34) William Tholl, Evidence before the Standing Senate Committee on Social Affairs, Science and Technology, 31 May 2001, Issue 17.
(35) James Worrall, Why I will refuse to be a rural doctor, The Globe and Mail, 24 July 2001, p. A14.
(36) Ian Sempowski, M. Goodwin and R. Seguin, Physicians who stay versus physicians who go: results of a cross-sectional survey of Ontario rural physicians, Canadian Journal of Rural Medicine, Vol. 7, No. 3, Summer 2002, pp. 173-179.
(37) Morris L. Barer and G. L. Stoddart, Improving Access to Needed Medical Services in Rural and Remote Canadian Communities: Recruitment and Retention Revisited, paper prepared for the Federal/Provincial/Territorial Advisory Committee on Health Human Resources, Centre for Health Services and Policy Research, 1999, p. 3.
(38) Ibid., p. 4.
(39) Morris L. Barer and L. Wood, Common Problems, Different Solutions: Learning from International Approaches to Improving Medical Services Access for Underserved Populations, Dalhousie Law Journal, Vol. 20, Fall 1997, p. 324. Of course, provincial/territorial policies do not all fall neatly into these four categories; in practice, there exists a good deal of overlap.
(40) Barer and Stoddart (1999), p. 11.
(41) Government of British Columbia, Ministry of Health Services, Rural Programs 02/04: A Guide for Rural Physician Programs in British Columbia , p. 15.
(42) Government of Ontario, Ministry of Health and Long-Term Care.
(43) See, for instance, Barer and Stoddart (1999), p. 13.
(44) Morris L. Barer, L. Wood and D. G. Schneider, Toward Improved Access to Medical Services for Relatively Underserved Populations: Canadian Approaches, Foreign Lessons, Centre for Health Services and Policy Research, University of British Columbia, 1999, pp. 38-39.
(45) Tholl (31 May 2001).
(46) Peter Hutten-Czapski, Society of Rural Physicians of Canada, Evidence before the Standing Senate Committee on Social Affairs, Science and Technology, 31 May 2001, Issue 17.
(47) Iglesias (1999), p. 32. In 2001, the South African High Commissioner to Canada asked that Canada stop recruiting South African physicians because they are needed at home.
(48) Tholl (31 May 2001).
(49) Standing Senate Committee on Social Affairs, Science and Technology, Volume Two: Current Trends and Future Challenges, The Health of Canadians The Federal Role, Interim Report, 2002, p. 106.
(50) Hutten-Czapski (2001), State of Rural Healthcare, p. 4.
(51) D. J. Manson, and T. Thornton, Workshop Summary of the British Columbia Rural and Remote Health Conference, University of Northern British Columbia, 2000.
(52) Renée Lyons and P. Gardner, Building a Strong Foundation for Rural and Remote Health Research in Canada, St. Johns Rural Health Research Forum Summary Notes, Canadian Institutes of Health Research, 2001, p. 5.
(53) Canadian Institutes of Health Research, Rock announces CIHR strategic initiatives in rural health research, 2001.
(54) Bruce Minore, J. Kulig, N. Stewart and G. Mack, Rural Health Research Training in Canada: Where Do We Stand? Centre for Rural and Northern Health Research, report prepared for the Rural Health Research Consortium, 2001, p. 1.
(55) Hutten-Czapski (31 May 2001), Evidence.
(56) Hutten-Czapski (2001), State of Rural Healthcare, p. 2.
(57) Peter Hutten-Czapski and A. D. Thurber, Who makes Canadas rural doctors? Canadian Journal of Rural Medicine, Vol. 7, No. 2, Spring 2002, Table 2.
(58) Anne Robinson, Family Medicine North: This is the life! Canadian Family Physician, Vol. 47, September 2001; and Hutten-Czapski and Thurber (2002), Table 2.
(59) Hutten-Czapski and Thurber (2002), Table 2.
INTERNATIONAL APPROACHES AND LESSONS(1)
UNITED STATES
Most observers agree that there are serious problems with geographical distribution among physicians in the United States. It has been estimated that approximately 20% of the U.S. population lives in rural areas, while only 9% of the nations physicians practise in rural communities.(2) For the most part, federal and state policy makers have relied on market forces to address the distribution issue, supplemented by various educational and financial incentive programs. Most activity has occurred at the state level and has been described as a piecemeal effort to respond to geographical problem areas and not a coherent strategy designed to rationalize the allocation of health resources to improve access.(3)
The general approach is to provide federal or state funding to areas identified as medically underserved or that have a health professional shortage. These areas are determined based primarily on physician to population ratios and, to a lesser extent, on the proportion of the population that is elderly, the proportion that is below the poverty line, the infant mortality rate, and other local need indicators. Regions must apply every three years to be considered either a medically underserved area or a health professional shortage area so that they may be eligible for funding. A region that does not apply, no matter how desperate its situation, is not eligible for funds.
The two primary incentive programs in the United States are the National Health Service Corps (NHSC) and the Medically Underserviced Area program. The intent of the Medically Underserviced Area program is to make funds available to eligible regions so that they can encourage the development of Health Maintenance Organizations (HMOs organizations that coordinate health care insurance, health care delivery and purchasing on behalf of their members) in the area. The NHSC, rooted in federal legislation, is designed to recruit and retain primary care physicians to, and in, underserved areas.(4) This is done through scholarships and loans in exchange for a mandatory return-for-service. However, according to recent empirical evaluations, the NHSC has had disappointing rates of success. A 1992 study showed that long-term (eight-year) retention percentages for NHSC physicians were only 12%, compared to 39% for physicians who had not gone through the NHSC program.(5) According to a 1993 study, about 60% of NHSC physicians had left their rural practice within four years of arrival.(6) These studies suggest that those physicians who choose to settle in health professional shortage areas tend to be more committed to rural area practice, and more likely to remain there, than those physicians attracted to such practices through a financial incentive program. Therefore, relying on financial incentives to encourage physicians to locate in such areas will leave governments far short of solving these problems.
LESSONS FOR CANADA FROM THE UNITED STATES
According to Barer, Wood and Schneider, it would seem that Canada might learn what not to do, rather than what to emulate, from the American experience. First, simply increasing physician supply and relying on market forces spillover of physicians into rural areas once urban areas become saturated does not resolve rural access problems. Second, financial incentives do little to attract physicians who are not committed to rural areas. Whether a Canadian version of the NHSC (the federal financial incentive program) would be helpful is difficult to ascertain. Such a program at the federal level might reduce competition among the provinces, but would likely infringe upon provincial constitutional jurisdiction in matters of health care.
AUSTRALIA
Australia, like Canada, has a relatively small population scattered over a large land mass. Moreover, Australia has struggled with similar challenges of physician distribution, having employed a mix of strategies similar to those in Canada. However, Australia has been extremely active in the education/training area. In 1992, the Commonwealth Government unveiled the first national strategy to address the undersupply of medical care in rural Australia. Major policies of the National Rural Health Strategy (NRHS) included funding for the General Practitioner Rural Incentives Program (GPRIP) intended to address recruitment and retention issues and the creation of the Australian Rural Health Research Institute, a consortium of five universities with rural campuses.
Policy discussions leading up to the creation of the NRHS identified two types of programs that might successfully address the long-term policy objective of providing a stable and acceptable level of physician services for residents of rural and remote areas. These long-term programs included initiatives that would:
1. Bring more students with rural backgrounds into medical schools; and
2. Provide more training in a rural setting to undergraduate and graduate medical students.
In support of the first initiative, $2.5 million was committed to medical schools in 1992, specifically to help with recruiting undergraduates from rural areas. A number of medical schools also altered entrance requirements so that rural applicants could be accepted with lower grades. In the most recent federal budget (2001-2002), funding was allocated to develop nine new rural clinical schools and three university departments of rural health, adding to an already existing national rural health education and training network that focuses on providing specific rural health training and encouraging medical and other health professionals to take up rural practice.(7)
LESSONS FOR CANADA FROM AUSTRALIA
Australia has been extremely active in the education/training area; there may be initiatives here of interest to Canadian policy makers. Rural health experts see Australias focus on the educational aspects as a promising strategy in helping to reduce the urban-rural health gap over the long term.(8) However, how much can one expect to achieve from education-related approaches? Despite a dedicated educational strategy, there are still barriers to providing reasonable access to primary care in many parts of rural Australia.
UNITED KINGDOM
Since the creation of the National Health Service (NHS) in 1948, the United Kingdom has always controlled the distribution of general practitioners through a negative direction policy. The central Medical Practices Committee is responsible for approving all General Practitioner (GP) applications for practise and has the power to refuse an application if the number already practising in an area is adequate (adequacy being determined by the length of patient rosters; any areas with average rosters of 1,700 patients or fewer per GP are restricted).
The U.K. also uses a number of financial policies. Initial practice allowances are paid to GPs who locate in designated areas. A second financial incentive involves attaching a deprivation payment to residents of deprived areas using an underprivileged area index, which considers factors such as the percentage of elderly people living alone, single-parent families, unemployed people, etc. GPs who serve patients from these areas receive a capitation supplement (ranging from US$15 to US$25) as an incentive to see patients from areas with these characteristics. One of the effects of using the underprivileged area index, however, is that deprivation payments often go to inner-city locations instead of rural areas, which may be more underserved. A number of other ad hoc inducement schemes provide physicians with a place of residence, surgery for rent, and locums (physicians who temporarily carry on the practice for an absent colleague) for annual and study leave, paid for by the health authority.
LESSONS FOR CANADA FROM THE UNITED KINGDOM
Overall, most observers agree that the U.K.s combination of central planning through the Medical Practices Committee and funding based on the number and type of patients on a physicians practice list has been relatively successful in addressing problems of geographic maldistribution of primary care physicians. In fact, health care researchers Barer, Wood, and Schneider argue that Canada could learn from the U.K.s balanced blend of administrative and financial incentives.(9) Yet, in Canada, a number of provinces have tried administrative policies similar to the U.K.s negative direction policy, only to be frustrated by constitutional and other legal challenges. It may prove difficult, therefore, to transplant these U.K. policy strategies onto Canadian soil.
(1) Much of this section is drawn from Barer, Wood and Schneider (1999), pp. 17-32.
(2) T. Konrad, The Problem of Shortages of Physicians and Other Health Professionals in Rural Areas: Empirical Evidence and Policy Recommendations, report prepared for the Council on Graduate Medical Education Workgroup on Health Professions Workforce Policy and Geographic Distribution, North Carolina; North Carolina Rural Health Research Program, University of North Carolina, 1996.
(3) D. H. Taylor, The Natural Life of Policy Indices: Geographical Problem Areas in the U.S. and U.K., Social Science and Medicine, Vol. 47, No. 6, 1998, p. 714.
(4) Note that these are not necessarily rural areas. A metropolitan area that applies and meets criteria may qualify as underserved.
(5) D. Pathman, D. R. Konrad and T. C. Ricketts, The Comparative Retention of National Health Service Corps and Other Rural Physicians, Journal of the American Medical Association, Vol. 268, No. 12, 1992, p. 1552.
(6) T. Konrad et al., The Rural HPSA Physician Retention Study, Agency for Health Care Policy and Research, University of North Carolina, 1993.
(7) Australian Department of Health and Ageing, Rural Health Policy Federal Budget, 2002.
(8) Hutten-Czapski (31 May 2001), Evidence.
(9) Barer, Wood and Schneider (1999), p. 21.